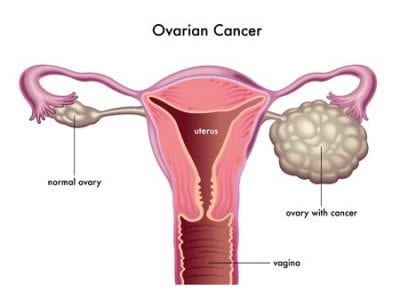
Ovarian Cancer is a disease that affects thousands of women annually. It ranks fifth in cancer deaths among women and accounts for more deaths than any other cancer of the reproductive system. The American Cancer Society predicts that in 2016, over twenty-two thousand women will receive a new diagnosis of ovarian cancer and over fourteen thousand women will die from it.
This cancer affects the entire reproductive system in the female body and can wreak havoc in a short amount of time. Older women are more prone to developing this form of cancer, over half being over the age of 63. The exact cause of ovarian cancers is not known, but there are many factors that improve the chances of getting them.
We also know that tubal ligation and hysterectomies lower the risk of ovarian cancer due to the fact that some cancer causing substances may enter the body through the vagina and pass thru the reproductive system to reach the fallopian tubes. A portion of ovarian cancers occur in women with inherited gene mutations that increase the risk.
These include mutations in the BRCA1 and BRCA2 genes, but some new research shows that early changes in fallopian tube cells increase the risk of developing ovarian cancer in over half the women that have these BRCA mutations.
Coming out of University College London, the study took post-surgical reproductive tissue from 115 women, 56 having either of the BRCA mutations and 59 that didn’t have the mutation. They found subcellular changes at either end of the fallopian tube in about sixty percent of those with the mutation that weren’t present in any of the women that don’t have the mutation.
Furthermore, the reprogramming of the cells at the proximal end of the fallopian tube in BRCA mutation carriers was driven by abnormally high levels of Activation-induced Cytosine Deaminase (AID) and could also be used in the early detection of ovarian cancer. Read more here: http://www.nature.com/ncomms/2016/160524/ncomms11620/full/ncomms11620.html
Last Updated on April 10, 2024.